We recently discussed the importance of nurturing a healthy gut. Gut health has been linked to many health issues including autoimmune disease, heart disease, mood, obesity, endocrine disorders, cancer, and more. When dysbiosis in the gut occurs, it can lead to further gut problems. This week we will be discussing in more depth gut health issues such as leaky gut, SIBO, and what you can do at home to optimize your gut microbiome.
. . .
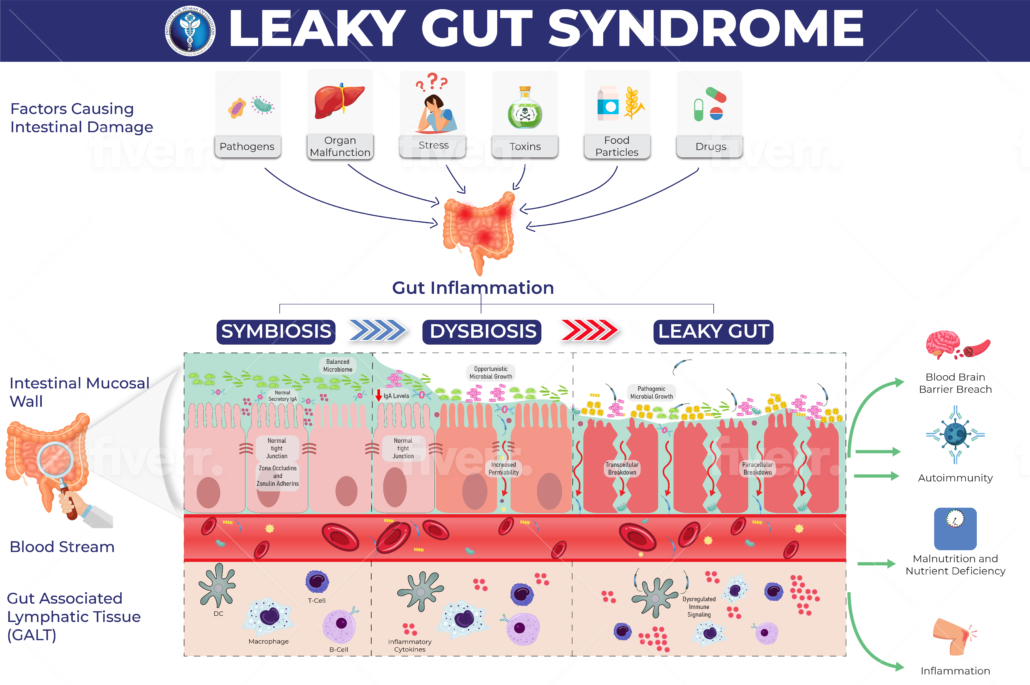
Leaky Gut Syndrome
The term “leaky gut” has been a buzz term on social media lately. In fact, leaky gut is a more recently known term within the conventional medical community. Leaky gut, also known as increased intestinal permeability, refers to when food particles and other things such as bacteria and toxins, “leak” through the intestinal wall that otherwise shouldn’t. Your gut is lined by the intestinal wall, think of it as a patio screen door. Ideally, the screen door in your home is free of damage providing a barrier from the outdoor elements from coming inside the house. The screen acts as a filter and allows only certain things of certain sizes to enter your home. However, if your screen door is damaged and/or has holes, over time it is easier for large bugs, debris, and other critters to enter your home. With time, the screen door is no longer functioning as a barrier. Similarly, in our gut when our intestinal wall is damaged, the small holes become larger which now allows for harmful substances to enter our system. Naturally, we all have some level of leaky gut as the barrier is a screen and therefore not completely impermeable.
What causes Leaky Gut Syndrome?
Your bio-individuality may make you more sensitive to changes in the digestive system, but your DNA does not determine your gut health destiny. Let’s look at a few common causes of leaky gut:
- Dysbiosis
- Diet
- Alcohol use
- Stress
- Food Allergies and Sensitivities
Dysbiosis
Dysbiosis occurs when pathogenic microbes (viruses, bacteria, mycobacteria) and symbiotic microbes that are beneficial to the microbiota by regulating our immune system, can no longer coexist in the gut in harmony. This is the leading cause of leaky gut syndrome.
Diet
A diet rich in processed foods or foods you are highly sensitive to (we will discuss this later) can lead to leaky gut. Unfortunately, I see more times than not how the American diet impacts patient health outcomes. Studies continuously show how ultra-processed foods adversely affect our gut microbiome which in turn, drives inflammation. The rationale is that the nutritional composition of ultra-processed foodstuffs can induce gut dysbiosis, promoting a pro-inflammatory response and consequently, a “leaky gut”.
Alcohol Use
Alcohol and its metabolites specifically promote intestinal inflammation through its influence on intestinal microbiota, immune function, and more. In large amounts, alcohol and its metabolites can overwhelm the gastrointestinal tract (GI) and liver and lead to damage both within the GI and in other organs. Alcohol disrupts the epithelial cells, cells that line the surfaces of your body, and disrupts the space between the cells which allows increased gut leakage.
Stress
Stress is a health disruptor on your body, mood, and behavior. In the case of leaky gut, it can increase gut barrier permeability which can result in “leaky gut”. There are many stress management strategies that you can try to incorporate from the comfort of your home such as physical activity, meditation, relaxing music, and yoga. If you are unsure where to start and/or have taken steps to manage your stress with no results, your healthcare provider can work with you to create a stress management care plan.
Food Allergies & Sensitivities
There is a difference between food allergies and food sensitivities. Food allergies are typically an acute hypersensitivity reaction that typically takes place within 2 hours of consuming the allergenic food. The symptomatic presentation can vary ranging from anaphylaxis, hives to respiratory or gastrointestinal distress. Food allergies are mediated by IgE immunoglobulin activity and cause a profound histamine release. Treatment can range from needing an epinephrine pen, steroids, and antihistamines. In contrast to Food Sensitivities, or intolerances which is typically more of a delayed hypersensitivity reaction which can take place upwards of 72 hours post-consumption which a varying symptomatic presentation which includes postprandial fatigue, migraines or body aches to common GI symptoms of gas, bloating, diarrhea or constipation. Food sensitivities are typically mediated by IgG and trigger inflammation. The problem is that foods that we are intolerant can present themselves very mildly compared to an allergy and cause chronic gut inflammation thereby increasing gut permeability. Additionally, it is important to keep in mind that 80% of our immune system resides in the digestive tract in the form of Gut Associated Lymphatic Tissue (GALT), and chronic exposure to larger food particles can ultimately lead to immunological programming and intolerances to foods that we commonly consume. Ultimately, this can trigger immunological dysregulation and autoimmunity.
SIBO
Another unassuming condition that often goes underdiagnosed and undetected is, Small Intestinal Bacterial Overgrowth (SIBO) occurs when excess bacteria are growing in the small intestine, disrupting the balance, and causing dysbiosis in your gut microbiome. Clinically, SIBO is an often-neglected mechanism for have patients presenting with weakened nutrition. Normally, you would find very little bacteria in the small intestine compared to the large intestine. SIBO has negative consequences on the structure and function of the small intestine and can cause mounting issues, including:
- Osteoporosis
- Kidney Stones
- Incomplete Digestion
- Vitamin Deficiency
Osteoporosis
Our bones are constantly undergoing continuous recycling throughout our lives. This process is known as bone remodelingand involves the removal of mineralized bone by osteoclasts followed by the formation of bone matrix through the osteoblasts that subsequently become mineralized. In other words, old bone is broken down and new bone is formed. For this to occur, our bones need a steady supply of protein, vitamins, minerals, and healthy fats to be properly absorbed. Healthy digestion is needed for optimal bone health. Over time, SIBO can cause poor calcium absorption which in turn drives bone loss.
Kidney Stones
If you know anyone who has had kidney stones, you’ve heard enough to hope you never have one. Kidney stones are a multifactorial complex disorder between the gut, liver, bone, and kidney. If you have SIBO, you have an increased risk of kidney stones because of the absorption issues that are a result of bacterial overgrowth.
Incomplete Digestion
Our small intestine continues the process of digestion that begins in the stomach and runs to your large intestine. But unlike the stomach, which has minor absorptive properties, 90% of food absorption occurs in the small intestine. Whatever is not absorbed is then passed on to the large intestine. Bacterial overgrowth disrupts conjugated bacterial cells, and dihydroxylation of bile salts, which are needed to digest fats, resulting in incomplete digestion of fats and diarrhea.
Vitamin Deficiency
The adverse effects of SIBO on nutrition involve several factors but one of the most common clinical manifestations is malabsorption. Vitamin B12 deficiency occurs in SIBO as the bacteria take up the vitamin. Vitamin A, D, and E are also commonly seen in SIBO due to the malabsorption of fat-soluble vitamins.
How can you optimize your Gut Health?
The health of our gut determines the health of the rest of our bodies. What are simple steps you can do at home to optimize your gut health?
- High Fiber Foods: Fiber has many benefits including lowering your risk for disease, regulates bowel movements, aids in weight management but also feeds your gut microbiome! The average fiber intake of adults in the United States is less than half recommended levels and is lower still among those who follow currently popular low-carbohydrate diets. Aim for your daily recommended amount from whole foods such as fruits, vegetables, seeds, and other plant foods.
- Reduce Stress
- Exercise Regularly
- Proper Sleep
At the Institute for Human Optimization, we understand that what starts in the gut impacts the entire body. No two patients are the same, so we work with you and create a personalized and individual approach to your gut health issues. What can that look like? Would you plant grass seed or kill the weeds first? Weeds should be killed first. Similarly, we will work directly with you to reduce or remove the weeds, aka factors that are driving dysbiosis. After that, we can work together to restore balance in your gut microbiome.
Disclaimer: The content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Additionally, the information provided in this blog, including but not limited to, text, graphics, images, and other material contained on this website, or in any linked materials, including but not limited to, text, graphics, images are not intended and should not be construed as medical advice and are for informational purposes only and should not be construed as medical advice. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition. Always seek the advice of your physician or other qualified health care provider with any questions you may have regarding a medical condition or treatment and before undertaking a new health care regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this or any website.

